
The therapeutic ketogenic diet is currently available to patients in most of the world (countries with known, established centers seen in black).
One goal of INKS is to make it available world-wide.
Partially Adapted from: Advancing the Awareness and Application of Ketogenic Therapies Globally: The Charlie Foundation for Ketogenic Therapies and Matthew’s Friends
By Beth Zupec-Kania, RD, CD, Jim Abrahams, Emma Williams, MBE, Susan A. Masino, PhD, and Jong M. Rho, MD
In: Masino SA, Boison D, D’Agostino DP, Kossoff EH, Rho JM (Eds). Ketogenic Diet and Metabolic Therapies: Expanded Roles in Health and Disease, 2nd Edition, Oxford University Press, 2022.

Overview
The Charlie Foundation for Ketogenic Diet was born out of the desire to spare children from the unnecessary suffering that Charlie Abrahams endured before achieving seizure freedom with the ketogenic diet. Jim and Nancy Abrahams shared their story in 1994 on Dateline NBC and later through a 1997 television movie called “First Do No Harm”. Across the Atlantic in the United Kingdom, Matthew Williams suffered for 6 years with a devastating seizure disorder before becoming practically seizure-free within 2 weeks of starting the diet.
show more
show less
Genesis of the Charlie Foundation
Charlie Abrahams, the youngest in a family of three children, had no apparent health problems until his first birthday in March 1993, when he experienced his first seizure. This was followed by a series of tumultuous events that changed his life as well as the lives of his siblings, Joseph and Jamie; his parents, Jim and Nancy; and ultimately thousands (possibly millions) of others. His father Jim described those months as follows:
show more
Charlie lived that period in his bed, on a blanket, or in an infant seat, where he was safely padded during the violent seizures that caused him to thrash uncontrollably. The adverse effects of the antiseizure medications were nearly as destructive as the seizures themselves. Between seizures, he was groggy, chronically constipated, and in the words of his father, seemingly “drunk.” Charlie also underwent a high-risk brain surgery to attempt to remove the area of the brain suspected to be the source of his seizures. He experienced zero improvement, and the seizures continued unabated.
Exhausted by the failure of the medical community to provide an effective therapy and reeling from the severe disruption inflicted on the rest of the family, Jim began looking for another option. He spent countless hours in the medical library at UCLA reading through literature on epilepsy, and it was there that he came across an epilepsy book containing a chapter on ketogenic diet as a treatment for epilepsy. He subsequently discovered a 1992 study from Johns Hopkins University that had been published in Epilepsia documenting 29% seizure freedom with an additional 30% significant improvement in 58 consecutive cases of children who were placed on a ketogenic diet (Kinsman et al., 1992). Notably, these children were as compromised by their disease as Charlie. Jim brought this book and the study to Charlie’s pediatric neurologist. Although Charlie’s neurologist was aware of the diet, he immediately dismissed it as a treatment that “he had never seen work.” Despite this discouragement, Jim and Nancy made the fateful decision to take Charlie to Johns Hopkins Hospital in Baltimore, Maryland. (At the time, Johns Hopkins was one of the few hospitals in the United States that had provided the ketogenic diet continuously since its discovery in 1921.) Dr. John Freeman and the dietitian Millicent Kelly formed the hospital team that implemented Charlie’s ketogenic diet.
Within 3 days of starting this treatment, Charlie was seizure-free. Over the course of the following month he was weaned off the four failed anti-seizure medications. Free from the sedating effects of those drugs, Charlie could finally hold his head up and once again interact with his family. Although the diet required careful measurements of specific foods, Jim described this as a “walk on the beach” when compared with their previous circumstances. This abrupt and almost incomprehensible reversal left the Abrahams with a diverse range of emotions; exhilaration and gratitude over Charlie’s sudden recovery was mixed with anger over the 9 months of unnecessary suffering that his son had endured.
Jim and Nancy appeared on NBC-TVs Dateline in 1994 to recap those months. They soon found their mailbox overflowing with letters from other families, thanking them for bringing the diet out into the light of day. Each letter described a similar journey to the one the Abrahams experienced with Charlie. The names and ages of the kids were different, but the stories were the same. Uncontrolled seizures, multiple medications, trips to the emergency room, mounting medical bills, and a drugged, poorly functioning child experiencing a rapid decline. Adoption of the ketogenic diet was the common denominator, and, for some, their lifesaver.
Jim was compelled to use his professional skills as a movie producer/director and his connections in the industry to find ways to help more families learn about the diet. He wrote, directed, and produced a dramatization of the devastating impact epilepsy can have, and the potential for the diet to stop seizures when nothing else has helped. In 1997, this story aired in a made-for-TV film called “First Do No Harm”. The film starred Meryl Streep (who received a Humanitas Award for her performance), and the movie became a conduit for spreading the word about the ketogenic diet worldwide. Twenty-two years later, the Charlie Foundation continues to hear from people who learned about the diet through this movie. Despite the diet’s now 100-year history, many physicians first learn about the diet from the families of their patients.
The Abrahams founded the Charlie Foundation to Cure Pediatric Epilepsy in 1994. Funding was provided for public awareness and research in animal models. Videos were developed for families and medical professionals, and the Johns Hopkins team received financial support for a book, The Ketogenic Diet: A Treatment for Epilepsy (now in its 6th edition). Over the last two decades, the Charlie Foundation has organized educational conferences, maintained a website, and trained medical teams at countless hospitals worldwide.
show less
Genesis of Matthew’s Friends
Matthew Williams was born in 1994. He suffered from a catastrophic form of epilepsy called Dravet syndrome, and his seizures started when he was 9 months old. Like Charlie, his seizures were severe, frequent, and uncontrolled by medications. Emma, his mother, asked if Matthew could try the ketogenic diet when he was 2 years old; she was told the diet “didn’t work.” As none of the medications helped, she continued to ask periodically about the ketogenic diet and was given a variety of responses; she was told the diet was “too hard” and caused “terrible side effects.”
show more
When Matthew was 7, at a routine appointment Emma insisted on trying the diet—the only other option was new combinations of drugs that had already been proven ineffective and shown to cause terrible side effects in Matthew:
“The side effects of the medications were awful. He was on a considerable amount of medication and his quality of life was so poor already that it really could not have got any worse for any of us.”
Fortunately, there was a new option. Six years after Emma first asked about the ketogenic diet, Matthew and 144 other children with severe epilepsy were enrolled in a clinical research trial of the ketogenic diet spearheaded by Dr. Helen Cross at Great Ormond Street Hospital (GOSH), London, England (Neal et al., 2008). Within 2 weeks of starting the diet Matthew’s seizures had decreased by 90% and within 8 months he was off all medication. His behavior improved dramatically. Unfortunately, for Matthew, the damage had been done. Years of experiencing thousands of seizures had caused tremendous brain damage, had broken his family apart, and Emma was now a single mum to Matthew and his younger sister, Alice.
Inspired by Matthew and hoping she could spare other families from what they had endured, and especially to prevent others from lifelong disabilities, Emma started Matthew’s Friends in 2004—initially running the charity out of her kitchen. She, like Jim and Nancy Abrahams, was shocked and angry at the lack of information and the underutilization of the diet—even when Emma had asked about it years earlier! She was determined to raise awareness and access to the ketogenic diet.
show less
Ten Years of Accelerating and Complementary Efforts
The past 15 years have been a period of enormous growth and revitalization for the field of metabolic therapy and for both foundations. One of us (Beth Zupec-Kania), a registered dietitian and nutritionist, joined the Charlie Foundation in 2006 to develop resources and trainings for ketogenic therapies. She designed an online ketogenic diet calculator program (KetoDietCalculator.org), which allows nutritionists to efficiently create diets including meal plans, special recipes, and infant and feeding tube formulas.
show more
In 2007, the Charlie Foundation estimated that fewer than 15 of the 200 children’s hospitals in the United States had a ketogenic diet therapy program. Frustrated by this lack of progress, the Charlie Foundation commissioned a group of physicians and dietitians to collaborate on methods of providing ketogenic diets. Their report, published in 2009 in Epilepsia was titled “Optimal Clinical Management of Children Receiving the Ketogenic Diet: Recommendations of the International Ketogenic Diet Study Group” (Kossoff et al., 2009). This consensus statement became the cornerstone for developing new programs worldwide. The report identified which patients were most likely to benefit, outlined methods of starting the diet, and provided monitoring guidelines. The group summarized its conclusions as follows:
“The ketogenic diet (KD) should be strongly considered in a child who has failed two to three anticonvulsant therapies, regardless of age or gender, and particularly in those with symptomatic generalized epilepsies. It can be considered the treatment of choice for two distinct disorders of brain metabolism, Glut-1 deficiency syndrome and Pyruvate Dehydrogenase Deficiency Disorder. In the particular epilepsy syndromes of Dravet syndrome, infantile spasms, myoclonic-astatic epilepsy, tuberous sclerosis complex, the KD could be offered earlier.”
Within the same year as this collaborative report, a randomized-controlled study of children receiving the classic and medium chain triglyceride-supplemented ketogenic diets was published in Lancet Neurology (Neal et al., 2008). This is the clinical trial in which Matthew Williams participated. Children between the ages of 2 and 16 with medically intractable epilepsy continued their current treatment and were randomized to either a ketogenic diet or standard of care for 3 months. The results were clear: children treated with the diet showed significant improvement compared with baseline and with the control group; some had over a 90% reduction in their seizures or were seizure-free. Seizure frequency in children who continued to receive the standard of care worsened compared with baseline, and none had over a 90% reduction or were seizure-free. This Class I study is considered the highest level of conclusive evidence and was the affirmation that doctors and advocates had been waiting for. At the time, it had been nearly 90 years since the ketogenic diet was developed and finally a comparison of the diet as treatment for difficult-to-control epilepsy against multiple anti-seizure medications proved that the diet was superior in effectiveness. More recently, another Class I study found similar results (Lambrechts et al., 2016).
The combination of the Epilepsia and Lancet Neurology publications gave further credence to the diet, and in 2010 led to the requirement for inclusion of ketogenic diet therapies in Level 3 and 4 Epilepsy Centers in the United States. This distinction is granted by the NAEC (National Association of Epilepsy Centers) to centers that provide medically approved epilepsy treatments.
show less
A Spectrum of Ketogenic Diet Therapies
Expanding use of the ketogenic diet for epilepsy paved the way to variations in the diet, particularly for adults and for older children who find it difficult to adhere to a restrictive diet. Dr. Eric Kossoff at Johns Hopkins developed a modified version of the ketogenic diet known as the modified Atkins diet (Kossoff et al., 2003). At about the same time, Heidi Pfeifer, a Massachusetts General Hospital dietitian, developed the low glycemic index treatment (LGIT; Pfeiffer and Thiele, 2005). These two newer diets are similar to the classic ketogenic diet in their high-fat, low-carbohydrate content, but are different in that they could be initiated outside of the hospital and do not require careful weighing of each food item.
show more
For now, the classic ketogenic diet remains the most effective diet therapy based on current scientific evidence. However, less strict versions may be more realistic for certain individuals, especially older children and adults. These metabolic diet treatments are referred to collectively as “ketogenic therapies.” The Charlie Foundation published a chart that outlines the differences between the therapies to assist families and health professionals in selecting the best option.
Both the Charlie Foundation and Matthew’s Friends offer a wealth of recipes and expertise, including demonstration videos. Their tireless dedication to developing and sharing recipes has helped make the diet enormously more palatable and accessible to patients and their families throughout the world.
show less
Other Conditions That May Benefit
A study published in 2008 in Lipids laid the groundwork for an entirely new application of ketogenic diet therapy. Metabolic syndrome is a diagnosis that includes three or more of the following abnormalities; abdominal obesity, elevated blood pressure, elevated fasting blood glucose, and elevated lipids or triglycerides. This syndrome is currently an epidemic in many areas of the world, including the United States and the United Kingdom. Improvements in metabolic syndrome were significantly better in a group that followed a modified ketogenic diet versus those who followed a low-fat, high-carbohydrate diet (Volek et al., 2008).
show more
People inquiring about ketogenic therapy for brain cancer have become the second-largest group (next to epilepsy sufferers and their families) requesting information from both organizations. These individuals often experience seizures; therefore, the role that the ketogenic diet offers as an antiseizure, anti-inflammatory, and antitumor therapy offers multifaceted benefits (Seyfried and Mukherjee, 2005; Veech, 2004). The ketogenic diet has also been shown to enhance the activity of a variety of anti-cancer therapies, reduce side effects, improve the anti-tumor immune response and reduce the formation of therapy resistance (Scheck and Syed, 2022). Several studies are currently in progress through the National Institutes of Health (NIH) investigating ketogenic diet effects on cancer. Recently, Matthews Friends has partnered with the Astro Brain Tumour Fund to help adults and children with brain cancer.
Additional applications of ketogenic diet therapies for other conditions have grown exponentially in recent years. Benefits have been reported in a multitude of neurological disorders and animal models of disorders including autism spectrum disorder, certain mitochondrial diseases, diabetes, migraine, Prader-Willi syndrome, neurodegenerative diseases including Alzheimer’s and Parkinson’s, multiple sclerosis, traumatic brain injury, stroke and mental illness. New research may expand the mission of the Charlie Foundation and Matthew’s Friends—or may bring new partners supporting metabolic therapies for diverse applications.
In response to the increasing demands for adult resources, the Charlie Foundation produced a guide in 2014 titled “Modified Ketogenic Therapy for Neurologic and Other Conditions.” Intended for use under medical supervision, it describes portion sizes for protein, fat, and carbohydrate and advice for optimal nutrition. The Charlie Foundation has shared resources with oncology medical professionals and expanded its website information to include this new population of users. A new link on the charliefoundation.org landing page has been added to ketogenic diet studies conducted through the NIH for cancer, epilepsy, and other disorders.
Medical supervision for ketogenic therapies and choosing the appropriate diet therapy for each patient is an evolving focus. The spectrum of therapies enables selection of the optimum diet for individuals, accounting for their overall health, diagnosis, age, and ability to comply. Matthew’s Friends developed a support system to help families prior to and during the diet to enhance the likelihood of success. Adjusting the therapy during treatment to optimize effectiveness is often necessary. Discontinuing the diet is usually the goal in childhood epilepsy: two to three years is the typical course of treatment. However, in some cases of epilepsy and other neurological disorders, it may be necessary to continue with a modified version of the diet indefinitely. These discussions are frequently addressed at the Charlie Foundation and have become the topics of collaborative journal articles and professional guidelines spearheaded by nutritionists.
News of ketogenic diet therapies has spread quickly through social media and the popular press. Thousands of copies of the Charlie Foundation’s Parent’s Guide to the Ketogenic Diet have been distributed in English and Spanish. Consultant chef Dawn Martenz and nutritionist Beth Zupec-Kania have collaborated on a new cookbook, Keto Cookbook II (Demos Publications). Cooking videos of the most popular keto recipes have been added to the charliefoundation.org website, and posts of creative snacks and meals are added to the Facebook page regularly. In addition, an App is under development for the modified ketogenic diet. Similarly, Matthew’s Friends (www.matthewsfriends.org/) is dedicated to developing and publishing delicious keto-friendly meals, and has produced a wealth of information for both parents and professionals by way of printed booklets, information films and national and international conferences
Both the Charlie Foundation and Matthew’s Friends have been continuously supportive of research and have partnered in funding global symposia on ketogenic diets. They stay abreast of new research related to ketogenic diet therapies. A recent study in the journal Obesity (2015) showed dramatic improvements in the health of obese children in just 10 days after eliminating sugar in their diets (Lustig et al., 2016). The metabolic impact of a sugar-free diet is one element of ketogenic diets that can be undertaken by anyone without the need for medical supervision. Eliminating sugar can be a difficult task for most people and requires strong motivation. A 2007 study published in Neuroscience and Behavioral Reviews showed that rats that were fed sugar intermittently had behavior and neurochemical changes that resemble the effects of substance abuse (Avena et al., 2008). Eliminating refined (processed) foods is a second step that can be taken to improve one’s diet.
The Charlie Foundation has translated these and other similar research findings into pragmatic guidelines. A new publication, “Does What I Eat Affect My Epilepsy?”, outlines steps that can be taken to eliminate sugar and refined foods and to consume a mostly whole foods diet. This has been distributed widely (in English and Spanish) for all people with epilepsy regardless of their interest in ketogenic diet therapy.
For conditions that may benefit from ketogenic therapies, the Charlie Foundation designed a “Pre-Ketogenic Diet”. This document is distributed (free) to health professionals to provide to their patients or clients who are potential candidates for ketogenic diet therapy. It recommends the elimination of gluten and sugar, in keeping with the classic ketogenic diet; however, it is not intended to induce ketosis. Instead, it can be described as a whole foods, Mediterranean-style diet that prepares the user for the transition to ketogenic therapy and also helps determine which diet in the spectrum is best suited for their needs and preferences. In addition, healthcare professionals can use the “Pre-Ketogenic Diet” as a screening tool to identify which individuals are able to adhere to the lifestyle changes required for ketogenic diets.
show less
The Charlie Foundation and Matthew’s Friends—Looking to the Future
In 2013, the Charlie Foundation renamed itself the Charlie Foundation for Ketogenic Therapies to better define its mission for the future: advocacy, awareness, and education for epilepsy and beyond. An expansion of education efforts includes adult-focused media and training. Development of new resources in both English and Spanish remains a goal. A list of current resources is shown on their web site.
show more
Throughout the 22 years of its existence, the Charlie Foundation has continued to receive daily e-mails and letters from families and health professionals requesting assistance. Jim Abrahams has responded to most of these requests himself, and triaging some to support staff. Although Charlie has been seizure- and drug-free and completely off the diet since 1999, Charlie’s family continues to represent ketogenic therapies in their Los Angeles community and on a national level through partnerships with other nonprofits and with supportive commercial organizations. Over 160 medical centers have been trained in the spectrum of ketogenic therapies in the United States and elsewhere, including Canada, Portugal, Austria, Jamaica, Slovenia, Kuwait, Saudi Arabia, and the Republic of Georgia. Beginning in 2008, the Charlie Foundation has also sponsored and organized global symposia which have brought together leading scientists and medical professionals with the intent of advancing research and clinical use of ketogenic therapies. Plans for future symposia are currently in progress. As new clinical and scientific research continues to emerge, both the Charlie Foundation will respond with further resources to promote safe and effective use of ketogenic therapies and make it less daunting for the user to manage.
Matthew’s Friends grew rapidly from Emma’s kitchen table and in 2011 opened its own clinic based at the Young Epilepsy site near London, treating children and adults with drug-resistant epilepsy. This continued for a period of 10 years, providing support to the under-funded NHS dietetic services. The charity expanded into New Zealand, Canada, South Africa and more recently to the Netherlands/Flanders. KetoCollege was launched in 2016, an in-person (UK) meeting offering CPD training for teams new to KD. This has expanded to on-line eLearning tutorials, free hot-topic webinars and more recently (2022) KetoCollege Advance in-person meetings for experienced KD teams, led by international experts in the field.
No longer on a special diet—Charlie Abrahams and Matthew Williams are two clear examples that even catastrophic epilepsy can be managed or even cured in some cases by a ketogenic diet. A question frequently asked about Charlie, Matthew, and others who have become seizure-free or nearly so on a ketogenic therapy is “How is it possible that they can retain the benefits after weaning off of the diet?” At the present time, there is no clear answer to this question. Emerging scientific research may soon clarify whether early application of ketogenic therapy may either ameliorate the disease or even cure it. For example, the field of nutritional genomics examines the effect of nutritional changes on genes and suggests that maladaptive epigenetic changes can be altered by diet. Targeted diet therapies are already being prescribed along with genetic testing for certain metabolic disorders.
Implementation of a restrictive diet is easiest in infants and children (given their reliance on the parents) and becomes more challenging as children gain independence. Early initiation of ketogenic therapies is better tolerated in young children—which may result in improved compliance and outcomes. Nevertheless, the diet has been shown to work in adults, and so in this light, future potential applications will continue to expand.
show less
Epilogue
Diet and nutrition can profoundly influence brain development and function. Indeed, from a medical perspective, dietary and metabolic therapies have been and continue to be explored in a wide variety of neurological diseases, including epilepsy, autism spectrum disorder, traumatic brain and spinal cord injury, Alzheimer disease, Parkinson disease, sleep disorders, malignant brain cancer, headache and chronic pain syndromes, as well as multiple sclerosis. More recently, a parallel approach has been taken to treat mental health disorders such as depression, anxiety, bipolar disorder and even schizophrenia. The impetus for using various diets to treat these disorders stems from both a relative lack of effectiveness of existing pharmacological therapies for many medical conditions and the intrinsic appeal of implementing non-pharmacological treatments.
show more
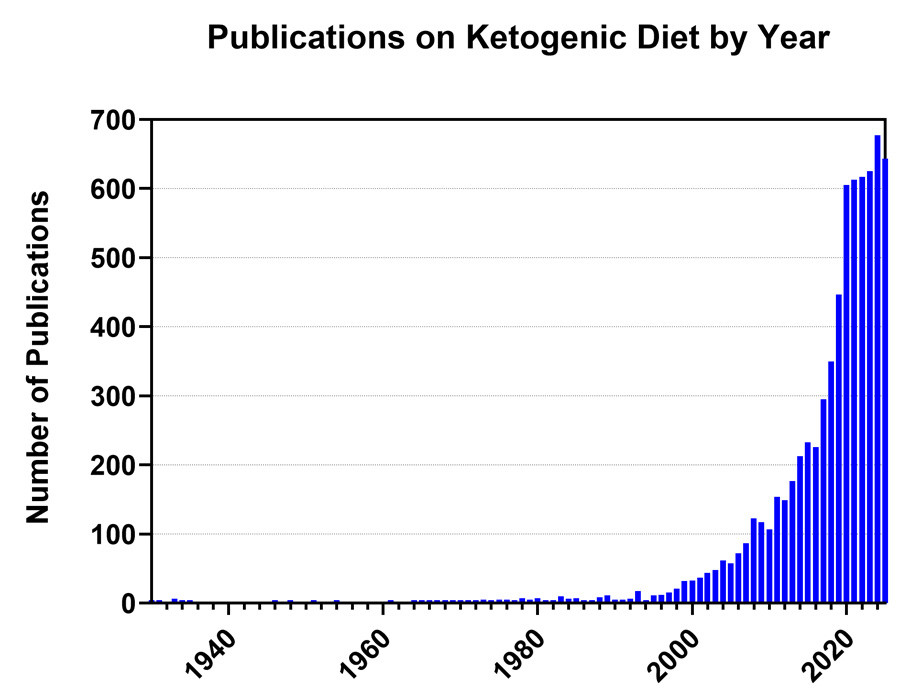
Over the past 25 years, the metabolic underpinnings of diseases that affect highly energy-dependent organs such as the brain have garnered widespread global interest and scientific validation. The catalyst for this exponential surge of activity was the Ketogenic Diet, a high-fat and low-carbohydrate treatment for pharmaco-resistant epilepsy which was created a century ago to mirror the biochemical changes induced by fasting – a strategy noted over two millennia to control seizures. While there have been great advances in our scientific understanding of how the Ketogenic Diet works over the last generation, one of the more noteworthy observations has been that this metabolism-based approach affords neuroprotective and potentially disease-modifying effects – not simply symptom relief. Thus, there is now a timely opportunity to fully exploit these advances for the benefit of patients across the age-span.
Since 2017, medical professionals and non-profit organizations representing six continents on Earth have convened regularly to create a new global society devoted to the advancement of metabolism-based therapies for neurological disorders – from clinical, educational, research, training, community outreach and advocacy perspectives. This professional organization has been named the International Neurological Ketogenic Society or INKS, and its formal inauguration during the October 2021 Brighton (United Kingdom) Ketogenic Therapies Symposium coincided with the 100th Anniversary of the birth of the Ketogenic Diet. In parallel, regional global INKS Chapters will be created to establish a truly global network of centers and organizations whose mission will be to promote metabolism-based therapies for neurological and mental health disorders. While not all metabolism-based treatments result in prominent ketone body production, the term “ketogenic” has been retained to honor the historical origins of the rapidly growing fields fully embraced and supported by INKS.
For further information, please visit: globalketo.com and neuroketo.org
Susan A. Masino, PhD
Detlev Boison, PhD
Dominic D’Agostino, PhD
Eric H. Kossoff, MD
Jong M. Rho, MD
show less
References
Avena, N.M., Rada, P., and Hoebel, B.G. (2008). Evidence for sugar addiction: behavioral and neurochemical effects of intermittent, excessive sugar intake. Neurosci Biobehav Rev 32, 20–39.
Coppola, G., D’Aniello, A., Messana, T., Di Pasquale, F., della Corte, R., Pascotto, A., and Verrotti, A. (2011). Low glycemic index diet in children and young adults with refractory epilepsy: first Italian experience. Seizure 20, 526–528.
Karimzadeh, P., Sedighi, M., Beheshti, M., Azargashb, E., Ghofrani, M., and Abdollahe-Gorgi, F. (2014). Low glycemic index treatment in pediatric refractory epilepsy: the first Middle East report. Seizure 23, 570–572.
Kinsman, S.L., Vining, E.P., Quaskey, S.A., Mellits, D., and Freeman, J.M. (1992). Efficacy of the ketogenic diet for intractable seizure disorders: review of 58 cases. Epilepsia 33, 1132–1136.
Kossoff, E.H., Krauss, G.L., McGrogan, J.R., and Freeman, J.M. (2003). Efficacy of the Atkins diet as therapy for intractable epilepsy. Neurology 61, 1789–1791.
Kossoff, E.H., Zupec-Kania, B.A., Åmark, P.E., Ballaban-Gil, K.R., Bergqvist, A.G.C., Blackford, R., Buchhalter, J.R., Caraballo, R.H., Cross, J.H., Dahlin, M.G., et al. (2009). Optimal clinical management of children receiving the ketogenic diet: recommendations of the International Ketogenic Diet Study Group. Epilepsia 50, 304–317.
Lambrechts, D.A.J.E., de Kinderen, R.J.A., Vles, J.S.H., de Louw, A.J.A., Aldenkamp, A.P., and Majoie, H.J.M. (2016). A randomized controlled trial of the ketogenic diet in refractory childhood epilepsy. Acta Neuro Scand. doi: 10.1111/ane.12592
Lustig, R.H., Mulligan, K., Noworolski, S.M., Tai, V.W., Wen, M.J., Erkin-Cakmak, A., Gugliucci, A., and Schwarz, J.M. (2016). Isocaloric fructose restriction and metabolic improvement in children with obesity and metabolic syndrome. Obesity (Silver Spring) 24, 453–460.
Mohanraj, R., and Brodie, M.J. (2006). Diagnosing refractory epilepsy: response to sequential treatment schedules. Eur J Neurol 13, 277–282.
Neal, E.G., Chaffe, H., Schwartz, R.H., Lawson, M.S., Edwards, N., Fitzsimmons, G., Whitney, A., and Cross, J.H. (2008). The ketogenic diet for the treatment of childhood epilepsy: a randomised controlled trial. Lancet Neurol 7, 500–506.
Perucca, E., Gram, L., Avanzini, G., and Dulac, O. (1998). Antiepileptic drugs as a cause of worsening seizures. Epilepsia 39, 5-17.
Pfeiffer, H.H., and Thiele, E.A. (2005). Low-glycemic-index treatment: a liberalized ketogenic diet for treatment of intractable epilepsy. Neurology 65, 1810–1812.
Scheck, A.C. and Syed, N. (2022) Ketogenic diet as adjunctive therapy for malignant brain cancer. In: Masino SA, Boison D, D’Agostino DP, Kossoff EH, Rho JM (Eds). Ketogenic Diet and Metabolic Therapies: Expanded Roles in Health and Disease, 2nd Edition, Oxford University Press.
Seyfried, T.N., and Mukherjee, P. (2005). Targeting energy metabolism in brain cancer: review and hypothesis. Nutr Metab 2, 30.
Sharma, S., Sankhyan, N., Gulati, S., and Agarwala, A. (2013). Use of the modified Atkins diet for treatment of refractory childhood epilepsy: a randomized controlled trial. Epilepsia 54, 481–486.
Shorvon, S.D., and Reynolds, E.H.. (1979). Reduction in polypharmacy in epilepsy. Br J Clin Pharmacol 7, 413P.
Thibert, R.L., Pfeifer, H.H., Larson, A.M., Raby, A.R., Reynolds, A.A., Morgan, A.K., and Thiele, E.A. (2012). Low glycemic index treatment for seizures in Angelman syndrome. Epilepsia 53, 1498–1502.
Veech, R.L. (2004). The therapeutic implications of ketone bodies: the effects of ketone bodies in pathological conditions: ketosis, ketogenic diet, redox states, insulin resistance, and mitochondrial metabolism. Prostaglandins Leukot Essent Fatty Acids 70, 309–319.
Volek, J.S., Fernandez, M.L., Feinman, R.D., and Phinney, S.D. (2008). Dietary carbohydrate restriction induces a unique metabolic state positively affecting atherogenic dyslipidemia, fatty acid partitioning, and metabolic syndrome. Prog Lipid Res 47, 307–318.




